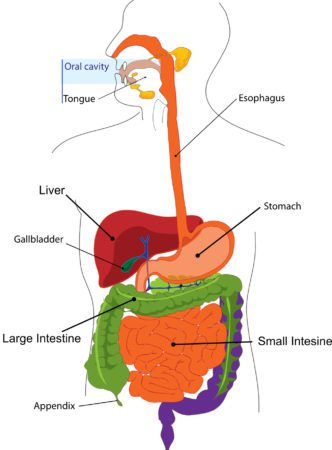
 The liver, located under the right rib cage, is the body’s largest internal organ and acts as a factory, regulating digestion, blood content, nutrient production and storage. The liver processes all that funnels through our bodies including what we consume as food and beverages through filtration and storage. The liver also rids harmful substances out and recirculates beneficial nutrients to other parts of our bodies. However, when the liver becomes damaged or injured, it cannot metabolize drugs, produce proteins used for blood clotting, filter blood, and aid in digestion to its fullest extent. Thankfully, the liver has the ability to regenerate itself to its full size (the only internal organ that can do so). Due to its immense functionality, liver health should be constantly monitored to ensure that its contributions to metabolic and chemical activity are not impaired.
The liver, located under the right rib cage, is the body’s largest internal organ and acts as a factory, regulating digestion, blood content, nutrient production and storage. The liver processes all that funnels through our bodies including what we consume as food and beverages through filtration and storage. The liver also rids harmful substances out and recirculates beneficial nutrients to other parts of our bodies. However, when the liver becomes damaged or injured, it cannot metabolize drugs, produce proteins used for blood clotting, filter blood, and aid in digestion to its fullest extent. Thankfully, the liver has the ability to regenerate itself to its full size (the only internal organ that can do so). Due to its immense functionality, liver health should be constantly monitored to ensure that its contributions to metabolic and chemical activity are not impaired.
As for GIST, all GIST-related medications are metabolized in the liver by the enzyme CYP3A4. GIST patients who are currently prescribed generic imatinib, branded Gleevec, Sutent, or Stivarga, should be aware of the associated liver health risks that may be caused by the medication.
Gleevec
Imatinib mesylate (Gleevec) targets several tyrosine kinases, such as Abl, KIT, and PDGFRs. It was found that hepatotoxicity, or injury to the liver, may occur while using Gleevec short-term and long-term. While taking Gleevec, liver function monitoring should be documented before and while taking the drug to review liver enzymes including alkaline phosphatase, transaminases, bilirubin, and albumin. In human microsome studies, Gleevec was found to be a potent competitive inhibitor for enzymes CYP2CP, CYP2D6, and CYP3A4/5, which play a role in the metabolism of imatinib. Although uncommon, severe liver toxicity, elevated liver enzymes, hepatocellular necrosis, and bile duct necrosis were found during long-term use animal studies. These adverse reactions are something to be aware of especially if you have other risk factors that have affected your liver health. (Source: Novartis Oncology: Gleevec Prescribing Information)
Sutent
Sunitinib malate (Sutent) remains a second line medication to imatinib mesylate (Gleevec) for gastrointestinal stromal tumor treatment. Currently, patients with unresectable or metastatic GIST with positive cKIT that are intolerant or become resistant to imatinib may commence Sutent. There have been several cases of liver injury attributed to sunitinib therapy, including hepatocellular blood enzyme elevations and acute hepatic necrosis. While some cases have come about due to direct hepatotoxicity, others may have been do to hypotension, shock or ischemia (restriction of blood supply to tissue). Sunitinib, like Gleevec, is largely known to metabolize via the CYP3A4 pathway in the liver. Within this chemical pathway, it has been noted that the production of a toxic intermediary molecule can also lead to liver injuries. Other risk factors to evaluate when considering starting Sutent are personal histories of known liver disease, alcohol use, or risk factors for viral hepatitis. (Source: National Institutes of Health: LiverTox Sunitinib Overview)
Stivarga
Clinically, regorafenib is used as a third line treatment option for progressive GIST once treated with imatinib mesylate and sunitinib malate. Regorafenib targets various intracellular and membrane-bound kinases, such as PDGFRAs, KIT, BRAFs and Abl. Stivarga was tested in terms of hepatobiliary disorders by Bayer. Bayer’s studies confirmed that Stivarga patients should routinely receive liver function testing. Increases in certain liver function biomarkers, like bilirubin, are listed on the most common side effects of Stivarga issued by Bayer. Bayer suggests a dose adjustment if severe liver impairment occurs. However, no dose adjustment is recommended in patients with mild or moderate hepatic impairment. Also, if Stivarga is taken with the co-administration of a strong CYP3A4 inhibitor, there seems to be a pattern with the reduction of active M-2 and M-5 metabolites which may increase the likelihood of increased toxicity. (Source: Bayer: Stivarga Prescribing Information)
Most of all liver injuries must be diagnosed by your physician. Therefore, it is highly recommended that you consult with your physician before, while and after taking GIST medications. While medication is not the only way to approach liver health, other changes in lifestyle and nutritional intake can improve liver functioning. It is important to monitor the liver, as it is known to be the most common site of metastasis in GIST patients. It is believed that because the liver filters blood, which can contain microscopic GIST cells, the liver’s environment can promote the survival and/or growth of tumor cells. Listed below are some suggestions to help protect your liver. In conjunction with medication, better daily habits, it is never too late to take preventative measures that can improve your overall health.
Lifestyle Changes:
- Limit alcohol consumption. There is a consensus that alcohol consumption, even in moderation, increases risk for cancer and recurrence in the gastrointestinal system.
- High stress levels and hormonal imbalances can compromise liver functionality.
- Incorporate different yet achievable forms of exercise daily like biking, walking, gardening, swimming, dancing, or yoga.
- Drink water to help the liver and kidneys eliminate toxins from your body. Adding lemon or lime can add flavor and antioxidants.
- Adding high-fiber foods, such as raspberries, broccoli, lentils, and whole grains can help to nourish healthy gut bacteria to remove toxins from the GI tract and ease the workload on the liver.
- Leafy greens have chlorophyll which plays a role in absorbing environmental toxins in the blood stream like chemicals, pesticides, and heavy metals.
- Add foods to your diet within the allium family, such as garlic, onions, shallots, and leeks, for their anti-inflammatory and antioxidant properties that support liver health.
- While taking Gleevec, Sutent and Stivarga, avoid grapefruits or grapefruit juices because they suppress the metabolic functioning of major liver enzymes.
- Herbal, vitamin/mineral, or botanical supplements can have 2-10 times the amount of nutrients found in food. A primarily plant-based diet, full of fruits, vegetables that vary in color is so much more beneficial.
Ask your physician:
- Speak to your physician if you are taking dietary supplements or herbs that may harm your liver.
- Ask your physician to test your liver enzymes and functionality.
- If suffering from liver enzyme elevation, consider dose reduction, temporary cessation, or a short course of Prednisone or Immuran.
- Be aware that certain medicines such as cholesterol-based drugs like acetaminophen (Tylenol), cold medicines, calcium blockers, and anti-depressive and/or anti-anxiety medications can damage your liver if taken too often.
While there is no evidence that changing your diet can protect your liver, the consensus is to keep a balanced diet and decrease alcohol consumption. As always, every individual’s case is unique; please consult your physician before making changes to your diet.
| Definitions | |
|---|---|
| Hepatotoxicity | The capacity of a drug, chemical or other exposure to produce injury to the liver |
| Necrosis | The death of most or all cells in an organ or tissue due to disease, injury, or failure of blood supply |
| Intermediary Molecules | Converted molecules or substrates during a metabolic pathway of biochemical reactions |
More Posts on Nutrition
Clinical Trials & Nutrition
Nutrition is important to keep in mind during any cancer treatment, but especially during a clinical trial.
Nutrition Management Webinar & Multidisciplinary Approaches in GIST
The Life Raft Group partnered with Fundación GIST México to present Nutrition Management and Multidisciplinary Approaches in GIST for GIST patients and caretakers on March 16th at 12pm ET.
Efectos de la Nutrición y la Microbiota Intestinal en pacientes con GIST
TE INVITA A LA REUNIÓN DE PACIENTES PARA CONVERSAR SOBRE:"Efectos de la Nutrición y la Microbiota Intestinal en pacientes con GIST". La Sra. Carbajal-López describió los beneficios de una nutrición adecuada, la relación entre la nutrición y los procedimientos quirúrgicos, el vínculo entre el microbioma y el cáncer, y el ejercicio. 07 junio.
Effects of Nutrition and the Gut Microbiome in GIST Patients
The Life Raft Group partnered with Fundación GIST México to host “Effects of Nutrition and Gut Microbiome in GIST Patients” on May 4th, 2022, presented by Ms. Berenice Carbajal-López.
How to Balance Your Diet During the COVID-19 Pandemic
Nutritional status plays a very important role in the prevention and treatment of contagious and non-contagious diseases. In the frame of a health contingency, the use of strategies that strengthen our nutritional status and immune system is essential.
A Lively Liver: Monitoring Liver Health with GIST
The liver, located under the right rib cage, is the body’s largest internal organ and acts as a factory, regulating digestion, blood content, nutrient production and storage. The liver processes all that funnels through [...]






